A beautiful smile is often the first thing people notice about you. However, some suffer from dental conditions that prevents them from pursuing that strong, healthy, and perfect teeth.
Hypocalcification, a lesser-known yet significant dental issue, can have a significant impact on your oral health. The condition can turn a healthy tooth into a weakened, discolored, and decay-prone structure. In many cases, hypocalcification has led to tooth loss as it can no longer stay alive and healthy in the mouth.
But fear not, as understanding the condition and its causes can help you take preventive measures and seek the right treatment options. In the rest of this article, we will take a deep dive into hypocalcification, exploring its causes, symptoms, and the available treatment.
Whether you or someone you know is affected by hypocalcification of teeth, this article will provide you with the much needed information and guidance to help you maintain a confident and dazzling smile.
Understanding Hypocalcification
Hypocalcification is a dental condition characterized by insufficient mineralization or calcification of the teeth, specifically the enamel. The tooth enamel is the outermost layer of a tooth and consist primarily of a mineral called hydroxyapatite. In normal tooth development, the minerals are deposited in a highly organized manner, creating a strong and durable enamel layer.
However, in cases of hypocalcification, mineralization of the tooth is disrupted, leading to areas of the enamel that have a reduced mineral content. This makes the affected tooth less dense, weaker, and more susceptible to damage.
Hypocalcification is contrasted against hypercalcification and enamel hypoplasia. Hypercalcification is a condition where there is excessive calcium deposited in the enamel while enamel hypoplasia is a defect that causes the enamel to form incompletely or incorrectly. Hypocalcification, hypercalcification, and enamel hypoplasia affects both baby teeth and adult (permanent) teeth.
Causes of It
There are several factors that can contribute to the development of hypocalcification.
- Genetic factors: Certain genetic conditions, such as amelogenesis imperfecta (AI), can affect the formation of enamel and lead to dental conditions such as hypocalcification. National Organization for Rare Disorders estimates that one in 14,000 to 16,000 children in the United States suffer from AI). Individuals with a family history of such genetic conditions are at a higher risk of developing hypocalcified teeth.
- Nutritional deficiencies: To ensure tooth development and mineralization, the teeth requires adequate intake of essential nutrients like calcium, vitamin D, and phosphorus. Insufficient consumption and absorption of these nutrients can result in hypocalcification. This is commonly observed in developing countries where nutritious food is not readily available.
- Fluoride deficiency: Fluoride plays a crucial role in the remineralization of teeth. However, deficiency of fluoride can contribute to hypocalcification and a weakened enamel.
- Medications: Certain medications taken during early childhood when the teeth are still developing can interfere with the proper formation of enamel and cause hypocalcification. For instance, the use of tetracycline antibiotics during tooth development can negatively impact enamel formation.
It is crucial that you identify the underlying cause of hypocalcification in order to address it effectively. However, some cases of hypocalcification may have no identifiable cause, and may be due to a combination of genetic and environmental factors.
Recognizing the Symptoms
The symptoms of hypocalcification can vary greatly depending on the severity and extent of the condition. Some common symptoms include:
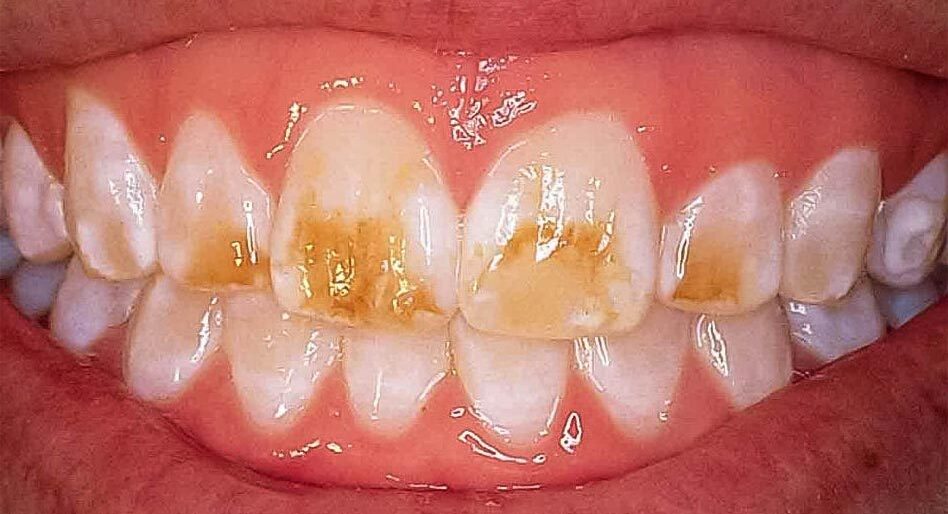
- Discoloration of enamel: Hypocalcification can cause the formation of white, yellowish, or brownish spots on the surface of the enamel surface. These spots may be small or large and can be located anywhere on the tooth surface. In some cases, the affected teeth may appear in a translucent form or have an irregular surface texture.
- Tooth sensitivity: When one suffers from hypocalcification, the weakened enamel can cause the underlying dentin to be exposed to the harsh environment of the mouth. This can cause the teeth to be particularly sensitive to an external stimulai such as hot, cold, spicy, sour, or acidic substances. Consumption of certain food and drinks such as carbonated drinks or hot food can cause tooth sensitivity.
- Chipping, cracking, or fractures: Teeth that are weakened by hypocalcification may be more susceptible to chipping, cracking, or fractures. This can quickly escalate into an infection as bacteria is able to penetrate the cracked tooth enamel and reach the dentin and dental pulp.
- Increased susceptibility to decay: Hypocalcified enamel is more prone to the effects of acid-producing bacteria in the mouth, leading to a higher risk of cavities and tooth decay.
- Frequent cavities: Hypocalcification can increase the risk of cavities and other dental problems. This is because the weakened enamel layer is more prone to decay and damage.
You may be interested in: Does Flossing Actually Whiten Your Teeth?
If you notice any of these symptoms happening, consult a dental professional as soon as possible to get a diagnosis. Early detection and treatment can prevent any further damage to the affected teeth and keep your overall oral health in check
Treat of Hypocalcification
The treatment for hypocalcification varies depending on the severity of the condition as well as the symptoms experienced. In mild cases, good oral hygiene practices may be sufficient to repair any damage done to the affected teeth. This includes the use of a fluoride tooth paste, regular brushing and flossing, and regular checkups with your dentist. Additionally, avoid a diet high in sugar or acidic food as it can aid the growth of bacteria and a weak acid in the mouth.
However, in more severe cases, dental procedures such as fillings, crowns, or even extractions may be required to restore or replace the damaged. Dental fillings are used to treat small cavities or areas of decay by filling the damaged area with a filling material. Crowns, on the other hand, are used to treat extensively damaged or decayed teeth by placing a tooth-shaped cap over the damaged tooth to protect it from further damage and decay.
In cases where a severely damaged or decayed tooth have been deemed by the dentist to be beyond repair, an extraction is necessary to prevent any infection from spreading to the surrounding teeth and gums.
An alternative form of treatment involves the use of fluoride, a mineral that can speeds up remineralization of the tooth. Fluoride work by combining calcium and phosphate ions together to form fluorapatite crystals on the tooth enamel, repairing parts of it that is lost by acid erosion. Fluoride treatment involves the application of a fluoride gel or varnish to the teeth, which is left in place for a period of time before being rinsed off.
Apart from treating hypocalcifcation, there is also a need to prevent decalcification of the teeth.
Takeaway
To sum up, hypocalcification is a dental condition that warrants attention as it can lead to problems such as a weakened enamel, tooth sensitivity, cavities, and even tooth loss. Early detection is key to addressing the condition effectively and preventing it from escalating into more severe dental issues.
There are several treatment options available for hypocalcification, ranging from good oral hygiene practices to more invasive dental procedures such as fillings, crowns, and extractions. Additionally, fluoride treatments can be a highly effective way to help remineralize and strengthen teeth against decay.
By staying informed and actively taking care of your oral health, you can deter hypocalcification and keep your smile shining bright for years to come.